By Drs. R. Pereira, A. Adams-Progar and D. Moore
What is the old saying? An ounce of prevention is worth a pound of cure? Are you using the ounce of prevention or the pound of cure? How about when a pound of cure can lead to antibiotic resistance and ineffective drugs?
Respiratory disease and diarrhea are the two most common illnesses that result in drug use in pre-weaned calves. Respiratory disease is commonly caused by both viruses and bacteria and usually requires antibiotic treatment. Diarrhea in pre-weaned calves is more common than respiratory disease and is most commonly caused by viruses (Rota and Corona) and protozoa (such as Cryptosporidium) that are not killed by antibiotics. Occasionally, diarrhea can also be caused by bacteria such as E. coli K-99 and Salmonella that require antibiotic treatment. Pinpointing if a calf with diarrhea needs treatment with antibiotics can be challenging when relying only on loose feces as a clue. This report will focus on tools that can help diagnose and choose the best interventions to treat calves with diarrhea effectively.
This publication is available for download from the WSU extension.
Consequences of diarrhea
When a calf has diarrhea, there are several consequences:
- The calf is losing fluids in the feces leading to dehydration.
- The calf is losing “strong cations” such as sodium, compared to strong anions such as chloride and lactate, creating metabolic acidosis.
- The calf may develop electrolyte imbalances because of losses of electrolytes in the feces.
- The calf will lose weight (due to less appetite or from not absorbing nutrients in the gut).
- There is the potential for overgrowth of gram-negative bacteria (like E. coli) in the small intestine.
- There is an increased chance for development of bacteremia (bacteria in the blood), particularly in calves with failure of passive transfer of immunity (those that may have or did not receive any or enough quality colostrum) and/or calves with severe diarrhea.
Not all these consequences happen in every case of diarrhea. Some calves simply have fluid and electrolyte losses, while others may have more severe clinical signs. The actual cause of death of diarrheic calves is not always known but likely includes dehydration and bacteremia/septicemia.
Use of antibiotics and antimicrobial resistance
Why should antibiotics be reserved for special cases of diarrhea? One consequence of non-selective use of a drug during diarrhea is the effect on calf health – a potential increase in the number of days of diarrhea. A study by Berge et al. (2009) observed that calves treated with antimicrobials for any case of diarrhea had 70% more total days with diarrhea than calves treated with antimicrobials only in cases of fever or depressed attitude. This can happen because antibiotics do not affect only disease-causing bacteria, they can also kill the normal gut microbes (which may protect against unwanted bacteria) and/or cause overgrowth of other bacteria, including drug-resistant, disease-causing ones.
Beyond therapeutic uses of antibiotics, feeding antibiotics to calves in the milk is a practice that has been and is still used by some for treatment and prevention of diarrhea in pre-weaned calves. Currently, feeding antibiotics in the milk or milk replacer is restricted in the U.S. to the first two weeks of life. However, this practice can result in an increased selection of drug-resistant bacteria and more days of diarrhea (Berge et al., 2009; Pereira et al., 2011) and the actual effectiveness of in-feed antibiotics for calves is questionable.
AMDUCA: What is extra label drug use?
- Use in species not listed on the label
- Use for indications (disease or other conditions) not listed on the label
- Use at dose, frequency, or route of administration other than those on the label, and deviation from labeled withdrawal
- Any extra label use of an approved drug must be prescribed by a veterinarian within the context of a veterinarian-client-patient relationship (VCPR)
A recent review of all the labeled drugs for prevention and treatment of diarrhea in calves revealed that none had consistently been shown fully effective (Smith, 2015). Because of that, treatment of calves with diarrhea may be done using drugs in an extra-label manner. According to the Animal Medicinal Drug Use Clarification Act (AMDUCA), extra label drug use in animals means the actual or intended use of a drug in an animal in a manner not in accordance with the approved labeling.
Extra label use of drugs should be avoided if possible because (1) it can increase selection pressure for resistant bacteria on the farm, (2) it may be illegal (depending upon which drug, for example, enrofloxacin is not approved for extra-label use in cattle), and (3) it may not result in a quicker cure. For some drugs such as ceftiofur (a third-generation cephalosporin antibiotic), the Food and Drug Administration has restricted extra label use conditions, which must be considered: “Veterinarians will still be able to use or prescribe cephalosporins for limited extra-label use in cattle … as long as they follow the dose, frequency, duration, and route of administration that is on the label.”
Due to potential disadvantages, use of antibiotics to treat diarrhea must be limited to targeted use. Based on a review of the literature (Constable, 2004), calves with diarrhea that have systemic signs of illness (poor appetite, dehydration, lethargy, or fever) or have blood in the feces have an increased risk of bacteremia (bacteria in the blood) and need antibiotic treatment. In these cases, administration of broad-spectrum beta-lactam antimicrobials (ceftiofur, amoxicillin, or ampicillin) is recommended. Developing skills to interpret severity of diarrhea in calves and choosing the most appropriate intervention is vital to improve treatment effectiveness.
Overall, indiscriminate use of antibiotics to treat diarrhea in calves can result in increased expenses with drug treatment, extend the length of disease and select for bacteria resistant to multiple drugs, including antibiotics important in human medicine. Selection of multidrug resistant bacteria, including non-pathogenic bacteria such as E. coli, can spread resistance to other bacteria on the farm and potentially increase the risk of drug-resistant infections.
What should calf treaters look for?
Understanding healthy calf behavior
How does a healthy calf spend its day? Before you can determine whether a calf is exhibiting abnormal behavior, it is important to understand how the average healthy calf would allocate its time each day (also known as a time budget). During its first six weeks of life, a healthy calf will spend 75% of its time each day lying and only about 4% of its time eating (Panivivat et al., 2004). Takeaway message – don’t ignore a calf that is exhibiting “normal” behavior for an abnormal amount of time.
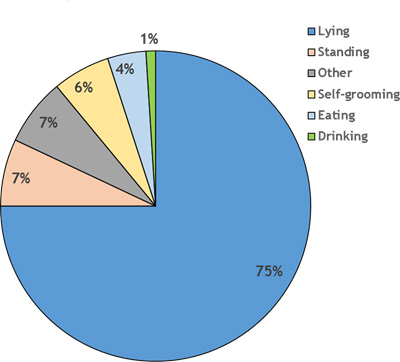
Healthy Calf Time Budget
Subtle behavioral differences, such as resting position, may also help you identify sick calves. A healthy calf will typically rest in a curled-up position with its head facing backward as it lies its head along its body. Pay attention to any calf that rests with its head facing forward and atop the bedding in front of its body (Moran, 2012). Healthy calves should be easily aroused, especially during feeding time, and will stretch when they stand after prolonged rest. Calf attitude is usually the first behavior evaluated to identify sick calves and is categorized as either alert (normal) or depressed (abnormal). A depressed calf lacks interest in its environment (including you), is slow to stand and eat (or refuses to eat), has a decreased milk drinking speed, and walks with a lowered head. Each calf responds differently to illness, so keep in mind that a sick calf may not exhibit all the behaviors associated with sickness.
When to start treatment
Early diagnosis and treatment of calves with diarrhea is vital for improving outcomes and reducing the need for antibiotics. The first step is to determine how sick the calf is:
- Can the calf stand? What is its attitude? (Is the calf suckling? Looks “bright and alert.”)
- If the calf can’t stand and does not have a good suckle reflex he is probably severely dehydrated and may be septic – this animal needs urgent treatment and examination by a veterinarian is highly recommended.
- If the calf can stand, its attitude and dehydration status will help determine how aggressive the treatment should be.
- What is the calf’s dehydration status?
- This can be done by taking your thumb and gently rolling down the bottom eyelid: Generally the bigger the gap between the eyelid and the eyeball (the more its “sunken” into the head), the more severe the dehydration. Under normal conditions, the eye should be right against the bottom eyelid.
- The skin pinch test can also be used: Pinch the calf’s skin to form a “tent,” and if the calf is normal, the skin tent will quickly go back into place. If the calf is dehydrated, the tent skin tent will take a longer time to return to normal.
- What do the feces look like?
- This can help estimate the speed of loss of electrolyte – the more watery the diarrhea, the greater the amount of liquids that are being lost or not absorbed.
- Does the calf have systemic signs of a bacterial infection (or septicemia)?
- Clinical signs that can be used to identify this include:
- Animals presenting fever (rectal temperatures above 103 -103.5 Cº)
- Blood observed in the feces
- Enlarged or swollen joints or navel
- Clinical signs that can be used to identify this include:
Some individuals may want to score the calves’ clinical signs for severity.
| Health status | Clinical signs | Score |
|---|---|---|
| Fecal | Formed | 0 |
| Semi-formed/soft | 1 | |
| Runny | 2 | |
| Watery | 3 | |
| Runny/watery with fecal blood | 4 | |
| Hydration | Normal appearance | 0 |
| Sunken eyes | 1 | |
| Skin tented 5-10 seconds | 2 | |
| Skin tented >10 seconds | 3 | |
| Attitude | Alert | 0 |
| Depressed | 1 |
Independent of the microbe causing the diarrhea, the first and most important steps in treating cases of calf diarrhea are:
- ALWAYS treat the dehydration first (See Smith and Berchtold, 2014, for specifics).
- Calves should always have access to water. If a calf is standing and has a good suckle reflex, oral electrolytes are recommended and if correctly chosen and administered will correct metabolic acidosis and electrolyte imbalance while keeping the abomasum pH low. Oral electrolytes should be given one to three times a day as needed.
- If a calf cannot stand and is severely dehydrated, intravenous fluids are needed and should be administered by a veterinarian or trained personnel.
- Calves presenting any of the clinical signs for systemic infections or septicemia are good candidates for using antibiotics to prevent or treat bacteremia and overgrowth of E. coli in the gut.
- Animals with fever may also be treated with an anti-inflammatory (such as flunixin meglumine or meloxicam). This can help improve appetite and suckling reflex.
How to measure treatment success
Although diarrhea can be evaluated using fecal scoring, improvement in fecal consistency is not a reliable guide to whether calves are hydrated and does not accurately reflect daily loss of water or electrolytes (Brooks et al., 1996). Fecal volume now does not reflect what is currently going on in the calf’s small intestine. Rehydration and correction of acidosis must focus on other clinical signs.
Measuring a successful outcome for treatment of diarrhea will vary according to the initial severity of clinical signs. Assessing dehydration through eye position or skin tent are good methods to evaluate improvement of rehydration therapy. For severe cases, improvement in attitude (standing and suckling) will help determine if treatment with antibiotics is working or if it is necessary. In addition, monitoring calf temperature is useful to evaluate treatment response in cases with signs of bacteremia and can help indicate if treatment with anti-inflammatories is needed or extended.
If no improvement is observed within two to three days, have the calf examined by the veterinarian. If clinical signs increase in severity, have the veterinarian examine the animal earlier.
Example of treatment considerations for a calf with diarrhea
Teaching new calf treaters may be easiest with use of a flow diagram. The following observations may be useful when explaining a procedure for evaluating calves for diarrhea. The very first observation might be that a calf did not finish its milk or milk replacer feeding. From that point, the calf treater might look at the feces and then the attitude of the calf and follow the flow chart:
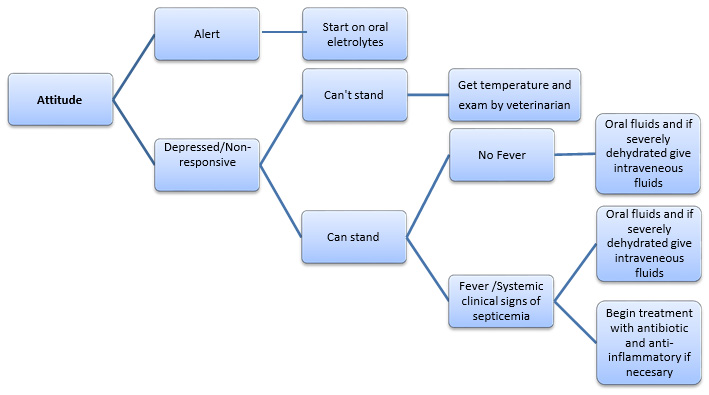
Specific, written treatment protocols are needed to address each treatment decision. These protocols should be written and understood by every member of the calf health care team. The availability of protocols to calf treaters is an important tool to avoid unnecessary or extra label use of antibiotics.
Prevention
Some tips for preventing diarrhea in calves require attention to cleanliness and provision of housing with adequate bedding and protection from the elements, resulting in a healthy and comfortable environment. In a study of calves and Salmonella shedding, Berge et al. (2006) found that calves housed in an open herd were over three times more likely to shed Salmonella than those in a closed herd.
A vital practice to increase resilience of the pre-weaned calf to disease is to feed newborn calves the proper volume (3 to 4 liters) of good quality colostrum (>60g of IgG/liter and <100,000 cfu/ml Total Plate Count) as soon as possible (within 4 hours) after birth. This will improve absorption of antibodies from the cow’s colostrum and secure a strong immune system. Failure of passive transfer of immunity through colostral immunoglobulins puts calves at risk for clinical disease.
Conclusions
Prevention is still the best approach to reduce occurrence of diarrhea and avoid unnecessary use of drugs. Monitoring and early diagnostics and treatment of diarrhea in calves is a key point to improve outcomes. Targeted use of antibiotics for treatment of diarrhea can reduce expenses with drug treatment, reduce length of disease (by avoiding unnecessary use) and decrease the risk of selecting multidrug-resistant bacteria, what can help extend the functional life of antibiotics in the farm.
References
- Berge ACB, Moore DA, Sischo WM, et al. Field trial evaluating the influence of prophylactic and therapeutic antimicrobial administration on antimicrobial resistance of fecal Escherichia coli in dairy calves. Appl Environ Microbiol. 2006;72:3872-3878.
- Berge ACB, Moore DA, Besser TE, Sischo WM. Targeting therapy to minimize antimicrobial use in preweaned calves: effects on health, growth, and treatment costs. J Dairy Sci. 2009; 92:4707-4714.
- Brooks HW, Michell AR, Wagstaff AJ, White DG. Fallibility of faecal consistency as a criterion of success in the evaluation oral fluid therapy for calf diarrhoea. Br Vet J. 1996;152:75-81.
- Constable P. Antimicrobial use in the treatment of calf diarrhea. J Vet Intern Med. 2004;18:8-17.
- Duse A, K Persson Waller, U Emanuelson, H Ericsson Unnerstad, Y Persson, B Bengtsson. Risk factors for antimicrobial resistance in fecal Escherichia coli from preweaned dairy calves. J Dairy Sci. 2015;98:500-516.
- Moran JB. Rearing young stock on tropical dairy farms in Asia. 2012. CSIRO Publications, Melbourne, Australia.
- Panivivat R, EB Kegley, JA Pennington, DW Kellogg, SL Krumpelman. Growth performance and health of dairy calves bedded with different types of materials. J Dairy Sci. 2004;87:3736-3745.
- Pereira RV, JD Siler, JC Ng, MA Davis, YT Grohn, LD Warnick. Effect of on-farm use of antimicrobial drugs on resistance in fecal Escherichia coli of pre-weaned dairy calves. J Dairy Sci. 2014;97:7644-7654.
- Raymond MJ, Whorle RD, Call DR. Assessment and promotion of judicious antibiotic use on dairy farms in Washington State. J Dairy Sci. 2006;89:3228-3240.
- Smith GW, Berchtold J. Fluid therapy in calves. Vet Clin Food Anim. 2014;30:409-427.
- Smith GW. Antimicrobial decision-making for enteric diseases of cattle. Vet Clin Food Anim. 2015;31:47-60.
The research and outreach for this WSU:Cornell project were supported by the Agriculture and Food Research Initiative Competitive Grant no. 2010-51110-21131 from the USDA National Institute of Food and Agriculture